TMJ | TMD Treatment in Pasadena and South Houston, TX
What is TMJ/TMD?
You think of your bite as your teeth, but a balanced bite actually requires the temporomandibular joint, the teeth, and the masseter muscles to all work together in harmony. When all is properly aligned, chewing is quiet and you don’t have pain in the jaw or lower face. But if one or more of the three components of your bite force the jaw into misalignment, you now have problems with every movement of the jaw. This can lead to pain across the jaw and face, and it can radiate down into the neck and shoulders. You are suffering from temporomandibular joint disorder (TMD).
You may have seen this denoted at TMJ, but that acronym refers to the temporomandibular joint itself. Proper identification of this group of related disorders that results from problems with the temporomandibular joint, the teeth, and the masseter muscles is a temporomandibular joint disorder or TMD.
Doctors or dentists who do not have specialized training with the temporomandibular joint and the corresponding disorder often misdiagnose the pain associated with TMD. Dr. Covell has pursued continuing education at the renowned Las Vegas Institute for Advanced Dental Studies to expand his ability to successfully treat TMD in his patients.
Call to Schedule Your Appointment
The difference between TMJ and TMD
As mentioned above, there is some confusion about the correct acronym to designate problems with the temporomandibular joint. You may have seen this disorder referred to as TMJ; you see it on our site as TMD. They can be used somewhat interchangeably, but there is actually a difference between the three.
- TMJ stands for the temporomandibular joint.
- TMD stands for problems with said joint, temporomandibular joint disorder.
- TMJD is not really used.
We use TMD when describing the condition at our Pasadena practice.
TMD Vs. bruxism
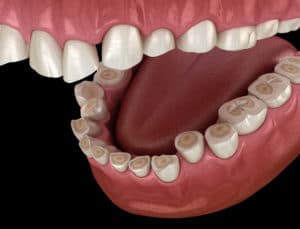
Bruxism, or teeth-grinding, occurs when the jaws are clenched and the teeth grind against one another. Stress and anxiety are often blamed, but sleep disorders, an abnormal bite, and missing or crooked teeth may also be caused. If left untreated, bruxism can lead to headaches, a sore jaw, or painful, loose or fractured teeth. It may sometimes lead to TMD. Click to learn more.
What Are The Symptoms Of TMD?
TMD can lead to chronic pain. It’s most common in younger people, between the ages of 20 and 40, occurring more in women than men. These are the typical symptoms associated with TMD:
Pain or tenderness in your face, jaw joint area, neck, and shoulders, or in and around the ears when you chew or otherwise open your mouth
- Jaws that get “stuck” or “lock” either open or closed
- Clicking, popping, or grating sounds in the jaw joint when you chew or simply open or close your mouth
- Consistent headaches
- Regular jaw stiffness
- Ear ringing (tinnitus)
- Unintentional teeth grinding
- A tired feeling in your face
- Upper shoulder pain
- Dizziness
Can temporomandibular joint disorder be misdiagnosed?
Temporomandibular joint disorder has only recently gained the attention it deserves. That’s because in the past the condition was often misdiagnosed as being due to other causes. Unfortunately, this is still the case with many dentists who don’t understand the TMJ and how it works, or in these cases, doesn’t.
A few other conditions can mimic TMD symptoms. Tooth decay, sinus problems, arthritis, and gum disease can all cause some of the symptoms we now associate with TMD. That’s why you need an expert, such as Dr. Covell, who is well-versed in understanding the differences.
The Causes Of TMD
Diagnosing TMD can be difficult unless the dentist has experience with neuromuscular dentistry, as Dr. Covell does. Symptoms such as earaches, headaches, and facial pain can be incorrectly attributed to sinus infections, tooth decay, even gum disease. Causes can be related to problems with the bite, but also from subtler issues such as stress and nightly teeth clenching during sleep. Traumatic injury to the jaw joints or related muscles can also lead to TMD. Some causes of TMD are still unknown, although research points to a possible genetic predisposition. Here are some causes of TMD:
- A misaligned bite between the upper and lower jaws
- Grinding or clenching the teeth
- Movement of the soft cushion or disc between the ball and socket of the joint
- Arthritis in the joint
- Stress, which can cause a person to tighten facial and jaw muscles or clench the teeth
- Injury to the jaw, head, or neck impacting the TMJ
- Missing or thoroughly worn teeth creating uneven biting surfaces
Can I develop TMD if I wear dentures?
Wearing dentures can actually cause TMD. That’s disconcerting but true. But it’s not the dentures, it’s the fit of the dentures that is the problem. If dentures aren’t properly fitted, you’re unable to maintain your bite. This leads to all the stresses of a misaligned bite that are behind TMD. Just because you’re using artificial teeth doesn’t change the fact that your jaw is out of alignment and is working with every movement to overcome the misalignment. That’s classic TMD.
Even if your dentures were correctly fit originally, they need to be relined, at most, every two years. This is because your jawbone deteriorates with the continuing use of dentures, so the fit changes. A reline will get the dentures back to proper fit and will alleviate the jaw alignment problems.
Can children develop TMD?
A child can be born with congenital jaw alignment problems that could lead to TMD, but this is quite rare. In the U.S., about 10 million people have TMD, with two-thirds of those being women. Symptoms usually first appear after puberty and peak between the ages of 20 and 40.
How does Dr. Covell diagnose TMD?
Dr. Covell has a good deal of experience with TMD, having received extensive continuing education in the condition at the prestigious Las Vegas Institute for Advanced Dental Studies. This is important, as many dentists and doctors attribute the signs and symptoms of TMD to other incorrect causes. In contrast, Dr. Covell has helped many of his Pasadena patients finally get the answers to their chronic pain whose root cause has been improper alignment and function of their temporomandibular joint.
When searching for a reason behind a patient’s jaw and neck pain, Dr. Covell first eliminates other conditions that can create the same symptoms: tooth decay, gum disease, arthritis, even sinus infections. From there he checks for areas of tenderness around the jaw joints. This is a sign that the muscles are being overworked. He’ll have you open and close your jaw, listening for the clicking, popping, and grating sounds typical with TMD.
We also use these tests to identify TMD:
- Full-face x-rays, MRIs, or CT scans — These may be used to view the position of the jaw and temporomandibular joints.
- Sonography – Sound waves are used to determine whether there are any problems with jaw alignment. Dr. Covell also listens for any abnormal sounds emanating from the jaw.
- Electromyography (EMG) – This method uses the electricity generated by jaw muscles to measure both muscle and nerve function. It can help to see when there is a reaction (such as pain) to movement.
- Computerized test equipment — This is used to measure the correct resting position of the jaw, identifying misalignment problems.
Call to Schedule Your Appointment
 How does Dr. Covell treat TMD?
How does Dr. Covell treat TMD?
In the majority of cases, TMD is treated with non-surgical methods. Dr. Covell usually seeks to ensure the patient’s jaw is in proper alignment before deciding on the course of treatment. His treatment approaches can involve everything from using anti-inflammatory medications to giving the patient exercises to do at home to help relieve stress on the TMJ.
Here are some of the methods Dr. Covell uses to treat TMD:
- Cosmetic dentistry — To correct alignment, we can replace missing teeth with dental implants or bridges, crown overly worn teeth, or move the teeth with orthodontics. This can involve widening constricted arches.
- Splints or night guards — Night grinding and clenching is often the main factor in TMD. To combat this, it’s important to put the jaw in the correct position at night. To do this, we fabricate plastic mouthpieces that fit over the upper and lower teeth. These are usually worn at night.
- Exercises — Tightening the jaw muscles and clenching the teeth is a common cause of TMD problems. We have various jaw exercises that stimulate and relax the jaw muscles.
- Medication — Muscle relaxants and anti-inflammatory medication can be effective.
- Lifestyle changes — Stress and anxiety are often root causes; stress reduction techniques are important.
- Transcutaneous electrical nerve stimulation (TENS) — Small electrical pulses are delivered to the jaw muscles through a small wand. These pulses stimulate the nerves, encouraging the muscles to relax and the jaw to fall into alignment.
Patient Testimonials
“A highly professional setting with the most current methods and practices. Appointment reminders via text and email are a huge plus. The staff is well trained and personable. Dr. Covell is highly skilled, comforting, and compassionate.“
– Harvey Price
“I was so nervous to look for a new dentist when I moved to Pasadena, and I am so happy that I’ve found Dr. Covell. He has the best chairside manner and really is a fabulous dentist. It’s amazing that he was able to meet with me on such short notice.”
– Nick Moore
Read more Patient Testimonials here.
Will Tmd go away if left untreated?

Exercises to help manage TMD pain
For some patients, exercises for the jaw can relieve their pain. These exercises seek to help by:
- Strengthening the jaw muscles
- Stretching the jaw muscles and TMJ
- Relaxing the jaw
- Increasing mobility
- Reducing jaw clicking
These are some exercises to try:
- Relaxed jaw exercise — Place you tongue on the roof of your mouth behind your front teeth. Consciously let your lower jaw relax downward, slightly separating your teeth.
- Goldfish exercises — Place an index finger in front of your ear where your TMJ is located. Put another finger on your chin. Open your jaw either halfway or all the way and feel the slight resistance.
- Chin tuck — Lightly link your hands behind your bottom to push your shoulders forward. Now pull your chin straight back as if you’re trying to create a double chin.
- Jaw resistance — Put your thumb under your chin and create some resistance as you open your mouth. Pinch your chin with forefingers and thumb of both hands to hold it when your mouth is open. Then close your mouth feeling the resistance.
- Tongue up — Hold your tongue up against the roof of your mouth, and then slowly open and close your mouth.
- Side-to-side and forward jaw movement — Place an object that’s about ¼ inch between your front teeth. First move your jaw slowly from side to side with the object between your teeth. Then do the same thing, but this time move your bottom jaw forward, so your bottom teeth are in front of your top teeth.
Can TMD affect other areas of the body?
The pain from TMD often spreads away from the jaw. Pain can encompass the entire face. From there it can affect the neck, shoulders, and even the arms. The ears can become tender. Headaches are typical. Tinnitus, or ringing in the ears, is common.
Will my dental insurance cover the diagnosis & treatment of TMD?
Awareness of TMD is increasing and insurance companies are finally recognizing the condition. Still, coverage varies depending on your carrier and your plan. Our team works with insurance companies to attain the most coverage, but it’s a good idea to do a little research with your provider beforehand to see what is or isn’t covered.
Why should I see Dr. Covell for my TMD?
Because TMD pain does spread out beyond the jaw, the source of the pain is often misunderstood, and more importantly, misdiagnosed by many dentists and doctors. Dr. Covell is very familiar with TMD and the operation of the temporomandibular joint. He has pursued extensive continuing education in this area of dentistry at the prestigious Las Vegas Institute for Advanced Dental Studies. He has a long history of treating patients in Pasadena and the surrounding areas and has reviews and testimonials from the patients he has helped get through their TMD.
Schedule a Consultation
If you’ve been diagnosed with TMD/TJ and you’re seeking professional treatment options for your condition, Dr. Paul Covell in Pasadena and Deer Park TX can recommend a treatment plan that will restore a healthier, happier mouth. Call his off at (713) 943-9832 or complete a contact form and someone will get back to you as soon as possible.

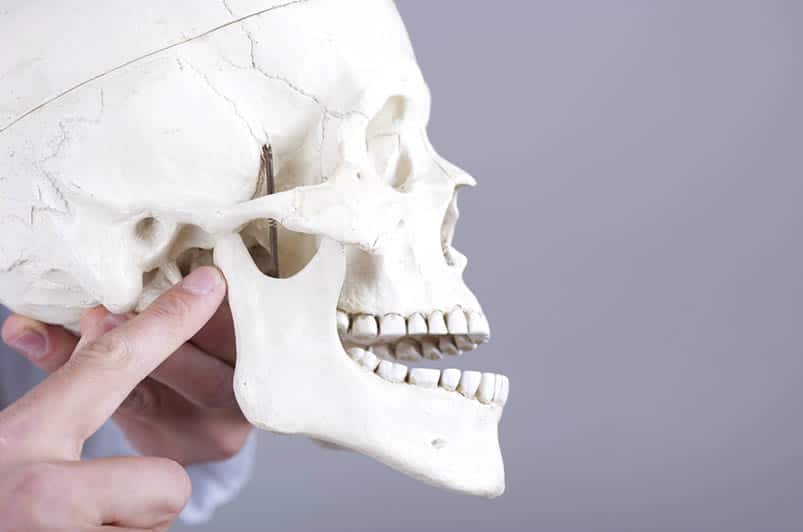
 Pain or tenderness in your face, jaw joint area, neck, and shoulders, or in and around the ears when you chew or otherwise open your mouth
Pain or tenderness in your face, jaw joint area, neck, and shoulders, or in and around the ears when you chew or otherwise open your mouth